Saturday, May 2, 2009
Tuesday, April 28, 2009
WHAT YOU SHOULD KNOW - KIDNEY CARE
![]()
 GET SCORED ON YOUR RISK FOR CHRONIC KIDNEY DISEASE!
GET SCORED ON YOUR RISK FOR CHRONIC KIDNEY DISEASE!
(a) I am ____ years old ?
Age: <50>
Score: 0 2 3 4
No Yes
(b) I am a woman 0 1
(c) I had / have anemia 0 1
(d) I have high blood pressure 0 1
(e) I am diabetics 0 1
(f) I have a history of heart attack or stroke 0 1
(g) I have a history of congestive heart failure 0 1
or heart failure
(h) I have circulation disease in my legs 0 1
(i) I have protein in my urine ( if unknown or
never cheked, score 0 ) 0 1
TOTAL SCORE _______________
Add up all the points. If you scored FOUR OR MORE POINTS, you have a one in five chance of having chronic kidney disease.
At your next doctor's visit, a simple blood test should be checked. Only professional health-care provider can determine for sure if you have kidney disease.
STEPS TO TAKE
1) Take only those medications, supplements, vitamins and minerals recommended by your doctor.
2) Ask your dietitian for help in planning your meals to get the right amount of nutrient and calorie intake when you are on a restricted protein diet.
3) Ask your dietitian for tips about flavouring your foods with herbs and spices in place of table salt.
Please keep in mind that KETO ACIDS Therapy has to meet the daily requirements for energy ( 30-35 kcal/kgBW/day).
If this is guaranteed, this dietary management not only avoids a shortage of essential amino acids but also keeps you in good nutrition shape.
Posted by BB at Tuesday, April 28, 2009 0 comments
WHAT YOU SHOULD KNOW
![]()
 Another Approach to " Kidney Care"
Another Approach to " Kidney Care"
ESSENTIAL KETO ACIDS FOR
RENAL NUTRITIONAL THERAPY IN
CHRONIC RENAL INSUFFICIENCY PATIENTS
HOW much do you KNOW?
1) Do you know what your kidneys can do for you?
- filter toxins and excess fluid ( cleaning the blood )
- helps in the making of red blood cells
- blood pressure regulator
- bone strength preserver
2) What are some of the risk factors contributing to kidney failure ?
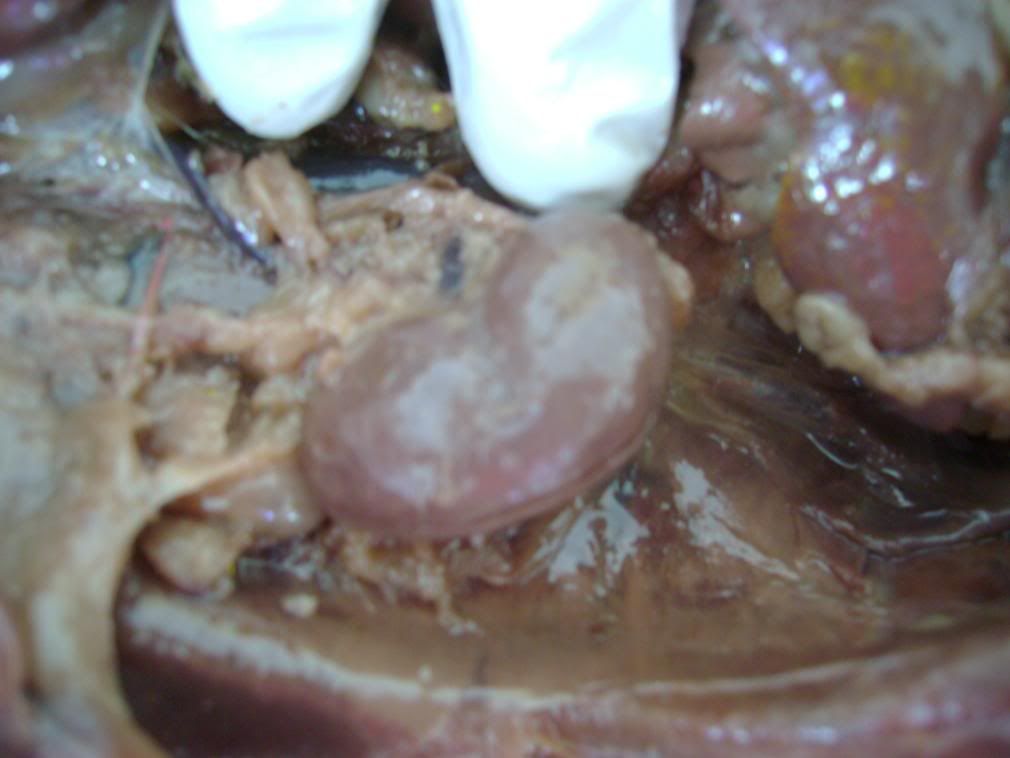
- Diabetes
- High blood pressure
- Kidney stones
- Nephritis ( inflmmation of the kidney )
- Family history
- Drugs
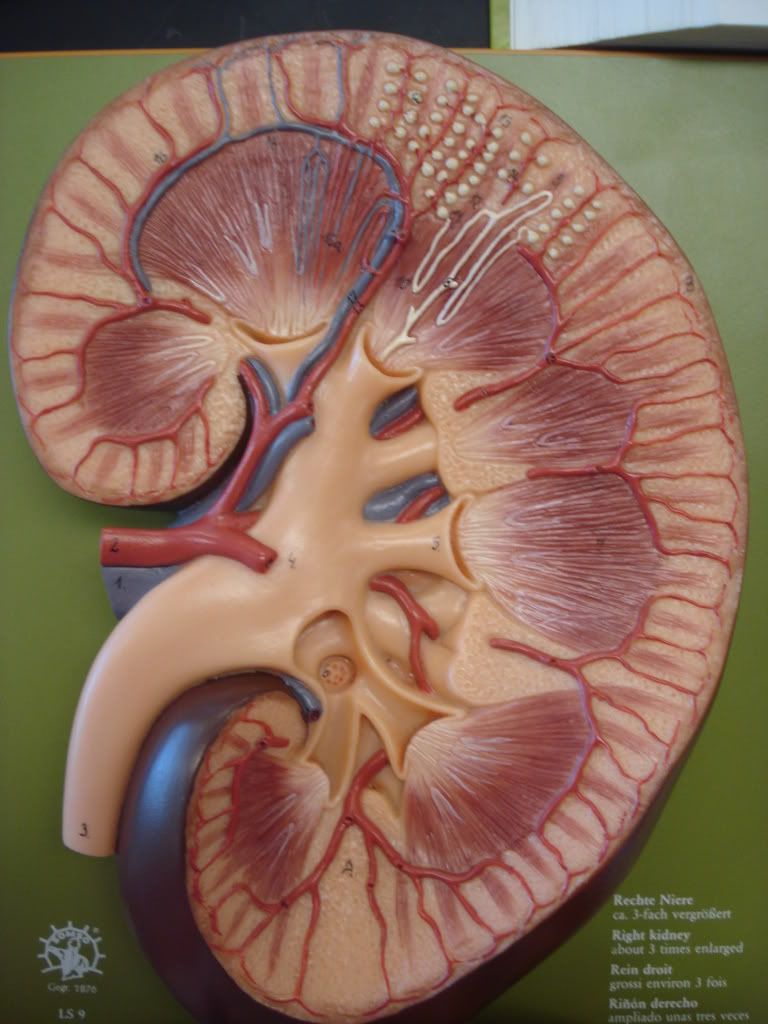 Chronic Kidney Disease ( CKD ) often presents no signs and symptoms in the initial phase
Chronic Kidney Disease ( CKD ) often presents no signs and symptoms in the initial phase
3) Do you know what are the signs and symptoms if they are present?
- tiredness
- reduced appetite, anorexia
- nausea and vomitting
- skin changes ( pigmentation, itchiness)
- swelling of the legs / face
- breathlessness on exertion
- anaemia ( lack of red blood cells)
 DO You Want to take Control of Your Kidney's HEALTH?
DO You Want to take Control of Your Kidney's HEALTH?
4) NUTRITIONAL THERAPY is an Early Interventional Method to delay the progression of kidney damage by the followings:
- minimize urine in the blood ( uraemic toxicity)
- avoid malnutrition
- delay End Stage Kidney Failure
5) What is NUTRITIONAL THERAPY ( KETO ACID THERAPY )
This involves controlling of protein intake from your diet with or without the supplementation of KETO ACIDS ( KAs ).
6) Why do you need to Restrict your Protein Intake?
- This is prevent the accumulation of waste products in the body.
- Reducing the dietary protein intake can help to reduce the workload on the already failing kidney and thus delay further kidney damage.
- Reduction of high protein intake is also associated with the reduction of phosphate, which then helps to preserve the bone composition.
EEA and KAs... WHAT ARE THEY?
7) Why do we need a supplementation of KETO ACIDS to our Restricted Protein Diet?
- There are 20 different amino acids available in our food that comes from protein. Some of these amino acids are called Essential Amino Acids ( EAAs ).
- EAAs are only obtainable from the food that we take and these are used by our body for daily protein synthesis ( i.e.blood, antibodies, muscles).
- By cutting down on our protein intake to avoid the accumulation of waste products in our body, we are risking a deficiency of some of these EAAs. Therefore, KETO ACIDS ( KAs ) are given to ensure our body is in an adequate nutrition state or is not malnourished.
8) What are KETO ACIDS ( KAs )?
- KETO ACIDS are nitrogen free precursor of EAAs ( will not generate waste products )and hence would not burden the kidneys.
- KETO ACIDS can also recycle the waste products in our bodies to from the necessary EAAs that our body needs and thus reduce the uraemic toxins.
Posted by BB at Tuesday, April 28, 2009 0 comments
Friday, April 10, 2009
Thursday, April 9, 2009
Monday, April 6, 2009
GENERAL INTENSIVE CARE UNIT
The General Intensive Care Unit of the Hospital is a level 1 ICU* that manages critically ill patients with complicated needs requiring the continuous availability of sophisticated equipment, specialized nurses and doctors trained in the care of the critically ill. The management of the unit is the responsibility of the Department of Anaesthesia & Intensive Care.
This document is prepared in view of the need for guidelines’ that would serve those who require the services of the Intensive Care Unit.
It is hoped that these guidelines would avoid the misuse or inappropriate use of facilities and staff and improve the utilization of scarce and costly resources.
These policies and guidelines would be reviewed and revised, as necessary, on a regular basis. Compliance with these guidelines will be monitored by the Department of Anaesthesia & Intensive Care.
* A Level 1 ICU is one capable of providing all forms of intensive care monitoring and therapy, have 24-hour access to diagnostic facilities, have dedicated medical staff roistered for 24 –hour duty and have a preponderance of nursing staff with intensive care certification.
ADMISSION AND DISCHARGE POLICY
An ICU provides services that include both intensive monitoring and intensive treatment. During times of high utilization and scarce beds, patients requiring intensive treatment ( Priority 1) have priority over patients requiring intensive monitoring ( Priority 2 ) and terminally or critically ill patients with a poor prognosis for recovery ( Priority 3 ). Eligibility for ICU admission and discharge is also based on reversibility of the clinical problems as well as the likely benefits of ICU treatment and expectation of recovery.
It is the responsibility of the patient’s attending doctor (or designee) to request ICU admission and to promptly transfer patients who meet discharge criteria.
It is to responsibility of the ICU specialist (or designee) to decide if the patient meets eligibility requirements for ICU.
In case of conflict regarding admission or discharge criteria, the ICU specialist (or designee) of the admitting unit will decide which patient should be given priority.
Admission Criteria
Priority 1
Critically ill, unstable patients with single system disorder and/or good reversibility of conditions and who require ventilatory support and/or continuous vasoactive drug infusion:
· Post-operative patients for stabilization and ventilation.
· Acute respiratory failure from a reversible cause e.g. Guillain-Barre Syndrome, Myasthenia Gravis, Bronchial Asthma, Drug Overdose.
· Patients with multiple trauma.
· Patients with acute obstetric complications e.g. post- partum haemorrhage, eclampsia.
Priority 2
Patients, who at the time of admission are not critically ill but whose condition requires intensive monitoring. These patients who are at risk for needing immediate intensive treatment would benefit from monitoring available in the ICU e.g. peripheral or pulmonary arterial monitoring, pulse oximetry.
· Patients with underlying hearts, lung or renal disease with acute exacerbation of the illness or the illness or who have undergone major surgery.
· Patients with progressive paralysis of neuromuscular origin
Some of these patients may be more suitable for High Dependency Ward admission. The underlying disease/s must be reversible or at least have a favourable outcome.
Priority 3
Critically ill, unstable patients whose previous state of health, underlying disease, or acute illness, either alone or in combination severely reduce the likelihood of recovery and benefits from ICU treatment,:
· Patients with metastatic malignancy complicated by infection.
· Patients with end-stage heart or lung disease complicated by a severe acute illness.
Patients who do not meet routine admission criteria are:
· Patients who have clinical evidence of brain death.
· *organ donors but only for the purpose of life support before organ donation.
· Patients with non-traumatic coma causing a permanent vegetative state.
Discharge Criteria
Priority 1 patients are discharged when their need for intensive treatment is no longer present.
Priority 2 patients are discharged when intensive monitoring has not resulted in aneed for intensive treatment and the need for intensive monitoring is no longer present.
Priority 3 patients are discharged when the need for intensive treatment is no longer present, but may be discharged earlier if continued is no longer present, but may be discharged earlier if continued treatment is futile or request for ICU bed for a Priority 1 or 2 patient is made.
Patients who are unlikely to benefit from continued ICU treatment include:
· Patients of advanced age with three or more organ system failures who have not responded to 72 hours or more of intensive therapy.
· Patients who are brain dead (*exception).
· Patients who have non-traumatic coma leading to a permanently vegetative state and a very low probability of meaningful recovery.
· Patients with protracted respiratory failure who have not responded to initial aggressive efforts and who are also suffering from haematologic malignancy.
· Patients with a variety of other diagnosis ( advanced chronic obstructive airway disease, end-stage cardiac disease or widespread carcinoma) who have failed to respond to ICU therapy, whose short term prognosis is also extremely poor and for whom no potential therapy exits to either the prognosis.
· Physiologically stable patients who are at low risk of requiring ICU treatment.
The least justifiable ICU activity on cost-benefit analysis lies in the management of diseases causing multi-system failure and a low survival rate in patients with short remaining lifespans.
The decision to discharge the patient will be made by the ICU specialist and the primary unit will be informed of this. The primary unit should then make arrangements for appropriate ward or intermediate care and promptly transfer the patient out of ICU.
The ICU SHOULD NOT be used as a High Dependency Ward. Nursing care in acute surgical wards should be upgraded to manage patients who require close monitoring.
TRIAGE IN THE ICU
Role Of ICU Specialist As Triage Officer
In times when patient load exceeds optimal operational capacity ( in terms of bed or ICU nurse availability ), there should be a clear policy as to who is responsible for triage within the unit.
The regulation of admission and discharge of patients into and out of ICU is a standard function assigned to the ICU specialist. However, another unenviable task of the latter is that of being a triage officer.
The triage officer should be a senior person who is knowledgeable about the prognosis of the various diseases related to the patients in the unit ( or able to obtain the information rapidly ), unbiased and a good negotiator. He / she must communicate directly with various primary attending doctors in order to identify any additional factors not readily apparent that might charge priority listing. He must not be overruled by other doctors during periods of high census.
The person best suited to make complex and dynamic triage decisions is the ICU specialist who has been regularly involved in the care of the patients.
Patients factors considered during high census :-
Functional outcome.
Chronic underlying condition (s)
Age .
Marginal benefit present.
Hospital mortality probability estimate.
Conditions defining limited medical suitability :-
DNR orders issued.
Patient considered unsalvageable clinically ( no marginal benefit)
Rapidly fatal underlying condition.
Persistent vegetative state.
High probability estimate of hospital mortality.
Triage Approach
To reduce inflow of patients to ICU
· Keep patient in Recovery bay, Casualty or other ICUs while queering to come to ICU.
· Hold transfer of patients from ICUs of other hospitals.
· Postpone high-risk elective surgery.
Increase performance of high census ICU
· Identify triage patient on daily basis such that patient can be promptly transferred when the need when arises. ICU Specialists should perform this together at a fixed time e.g.1500 hrs.
· Rapidly wean and extubate post-operative elective patient such that they are transferred out if stable for 4-6 hours after extubation.
Decrease workload per patient
Reducing nursing hours per patient by performing fewer invasive procedures e.g. deferring insertion of PAC.
Transfer to alternative sites
· Transfer the following patients to general wards.
· Patients who have failed aggressive ICU therapy.
· Patients who are considered unsalvageable.
· “Stable” ventilator-dependent patients.
· Transfer short-term recoverable patients to intermediate units e.g. other ICUs
· It is preferable such transfers be done during the daytime or on a scheduled or planned basis rather than late at night or as an emergency triage. Scale back orders before transferring.
*if all ICU beds in hospital are full, then the primary unit should seek permission from Director of Hospital to transfer patient to another hospital. (This is applicable to only Priority 1 patients who are citizens of Malaysia ).
BED REQUESTS FOR ELECTIVE SURGICAL CASES
The details of the patient and date of surgery will be documented on the ICU board.
The patient’s attending Surgeon/ Anaesthetist must inform and discuss with the ICU specialist in advance of the need for ICU Care for his post-operative patient.
In the event that there are more requests for ICU beds than beds available, than priority should be given to the following :
1. patient whose surgical condition is likely to deteriorate within days if surgery is postponed.
2. maternity patients.
3. patient whose surgery has been repeatedly postponed due to lack of ICU bed.
If a bed is not available for elective admission, the surgeon has the option of
1. Postponing surgery.
2. Arranging alternative ICU care within the hospital.
It must be emphassised that priority of admission will always be given to unscheduled, emergency admissions over scheduled elective requests.
WITHDRAWAL OF INTENSIVE THERAPY
The decision to withdraw therapy should be joint decision between the
1. Primary physician.
2. ICU specialist in-charge of the patient.
3. Designated senior specialist of the Department of Anaesthesia & Intensive Care.
The decision and rationale should be recorded in the medical record.
Intensive care therapies that are no longer indicated in such circumstances include:
CPR
Dialysis
Inotropes
Antibiotics
Parenteral nutrition
Therapy should be limited only to hygienic care and comfort.
The option to continue treatment for pain and suffering is available. Analgesics and anxiolytics may be used for this purpose.
The removal of life support from a patient should not be regarded as an abandonment of the patient by the healthcare team. Rather, the attention of the healthcare team must at this point be redirected to alleviating the suffering of the patient and his family and ensuring death comes with dignity.
PHYSICAL FACILITIES IN ICU
Bed requirements
Number of ICU beds per hospital should depend on type of services available in the hospital as well as the needs of the community.
Ranges from 2-6% of total number of hospital beds
working area about 200sq. ft/bed.
Open concept is highly preferred.
placing of bed in semi-circular position.
All patients can be viewed from the nursing station.
Windows located near the bed.
Day light in ICU.
Nursing station with central monitor ( optional ).
Sister’s office.
Male and female changing room with toilet and shower facilities.
Common rest rooms.
Treatment / preparation room.
Mini laboratory for essential test e.g. ABG, BUSE.
Sluice room.
Pantry.
Reception / conference room and library.
Waiting room for immediate family members.
Store room
Isolation room.
Doctor’s room.
Family waiting room.
BASIC EQUIPMENT FOR ICU
Basic monitoring equipment / bed
2 Electrocardiograph / Respiratory display
Pressure display – 2 to 3 channels
Temperature display
Pulse oximetry
Non-invasive blood pressure – adults, paediatrics and infants
Cardiac Output
12 Lead ECG monitor / recorder } to be available
Defibrillator – adult / paediatrics paddles }
Ventilators
High end to medium range ventilators for both adults and paediatrics patients.
Neonatal ventilators if ( admitting neonatal patients )
Sufficient number for all beds with spares.
Other Equipment
a) Manual resuscitation sets for adults, paediatrics and infants ( every bed – 1 set each )
b) Oxygen flowmeters (wall mounted humidification )
- Hot ( large volume nebulizers / cigar blower )
- Cold
c) suction regulators / wall mounted with high and low suction
d) syringe driver pump – 6 units / bed
e) transport monitors / ventilators
f) flexible fiberoptic scopes
g) essential airway equipment
Beds
Adult with facilities for:
- Positioning
- Resuscitation
- X-ray cassette placement
- Weighing
Paediatrics with facilities for:
- Central heating
- Phototherapy
- Oxygen / suction
- X-ray cassette placement
- Weighing facilities
- Apnoea alarms
Bedside facilities
i.Intravenous support system
ii.Railing for curtains
iii.Adjustable shelves for syringe pumps
iv.Railing systems for oxygen therapy and suction
v.Pendants or suitable mounting for monitors / IV lines.
vi.Adequate facilities for washing hands ( elbow control, hot and cold water )
Other requirements
a) Pipelines / outlet :-
3 Oxygen
2 Compressed Air
2 Vacuum ( 1 low and 1 high pressure )
b) Power
· 12 per bed with 6 UPS
· Emergency lighting – 2 power supply to all points
· Separate output for X-ray.
c) Cooling and heating devices
· Radiant heater
· Portable cooling mattress
d) Emergency trolley – 1 per cubicle
· Adults
· Paediatrics
e) Flooring
· Non-slippery surface
f) Furniture
· Table and chair ( for nursing staff ) for each bed.
g) X-ray
· Multiple viewing boxes for comparison of films
ICU BED SET UP
Monitor cables, arterial line, NIBP cuff and pulse oximeter.
Oxygen apparatus and resuscitation bag.
suction catheters of various sizes.
Writing table and chair.
Ventilator.
Resuscitation trolley.
Defibrillator.
ICU bed.
ORIENTATION OF NEW STAFF
ICU layout
staffing ; Roster :-
Checking of roster daily
Request
Annual leave
Emergency leave
Sick leave
Changing of duty
Attitudes ; Initiative :-
Acceptance of Correction
Work with rationale
Team work
Caring towards fellow staff, clients and relatives / visitors
Superiors
Keep up with current knowledge – reading, attending seminars or attending hospital’s CME.
Dress Code :- Scrub suit or apron , Cap and Mask during procedures
Documentation :- Admission Book, Census, Computers
Address Book – Home and contactable address and phone . numbers.
Incident Book/ forms :- POMR /OTHER/STUDIES.
Severity Scoring forms
Others :-“Fall Meja” , Circulars
ICU Nursing Care
ICU Charts / Admission – Treatment Charts
Monitors / Arterial line / CVP line
Ventilators :- Settings , Alarms , Changing of ventilatorcircuits/Humidifier , Resuscitation bags
Oxygen Apparatus
· Suction Apparatus :- Pressure Control , Changing of suction liners/tubings and catheters
· ICU bed :- Manipulation
Care Of ICU patients :- Observation and Documentation – General and local
· Personal care
· Participation :- General rounds , Procedures , Investigations , Transfer out/ discharge/ death /sending for CT Scan
· Treatment :- feeding , medication oral or injection , dressing
· care of relatives/visitors
· communication skills
· counseling skills
All care given to be planned, organized and priorities to be implemented according to client’s general condition and needs.
Ø VISITING HOURS
Generally all ICUs follow the hospital guidelines for visiting hours but special privileges are extended to the next-of-kin.
Each patient is allowed to have two visitors at any one time. For every patient that is admitted to General ICU, one visitor’s pass will be given to the next-of-kin. This pass allows 2 nearest family member to visit or stay in the hospital compound. They are allowed to visit the patient briefly during non-visiting hours. However they are not allowed in during doctors round, or during medical or nursing procedures.
Ø ADMISSIONS/ TRANSFER IN OF PATIENTS TO ICU
Ø TRANSFER OUT/DISCHARGE FROM ICU ( The receiving ward staff to each patient)
Ø DEATH IN ICU
· Contact next of kin/immediate family or inform police if unable to contact immediate families.
· Inform primary unit doctor regarding death and to be present in ICU to certify the cause of death and to sign burial permit.
· Do last office.
· 3 tags used. ( Red tag for police cases)
· If police case, to inform police.
· Ward attendant to get burial permit book.
· Documentation
- Admission book/ward census/record office census and computer.
- Report writing
sent body to mortuary
cleaning of bed unit.
Preparation of bed unit for next admission.
- A.. * Clinical post mortem – unit doctor to get consent from next-of-kin. ( BHT to sent to mortuary with body and document in mortuary dispatch book)
- B. * Body of organ transplant donor. Last office to be done by ICU staff in ICU.
Ø TRANSPORTATION OF VENTILATED PATIENT FROM ICU THERAPEUTIC PROCEDURES/ TRANSFER OUT TO SPECIALIZED UNIT.
Ø SENDING PATIENT FROM ICU TO OPERATION ROOM
Ø FETCHING PATIENT FROM OT TO ICU ( Patient from outside ICU ) ELECTIVE CASES / EMERGENCY CASES
Ø ROUTINE NURSING PROCEDURES IN ICU
To check individual nursing assignment of the day
Attend nursing handover report of allocated patient and the whole cubicle report.
Assess patient’s general condition :-
Level of consciousness , Colour , Pupil sizes , Vital signs
Report any significant changes to the ICU doctor.
Ventilator checking :- Settings , Alarms
Drug checking :- Perfusors : ( To check correct dosage and dilution )
a) Sedations
b) Relaxants
c) Inotropes
d) Antibiotics
e) Others
6. Nursing care plan
· Frequency of observation
· Special test
· Dressings
· Physiotherapy / suctioning
· Care of personal hygiene
· To note changes of ventilator settings
Routine observation
HOURLY
· BP / Heart rate / respiration ( continuous monitoring )
· Oxygenation (SpO2), ventilator settings
· Urine output
· Head chart
4 HOURLY
CVP reading
Temperature
Random Blood Sugar ( Dextrostix )
Urine Output
Ryles tube Aspiration
Head Chart
( The frequency of observation varies according to patient’s general condition and doctor’s orders )
DAILY & PRN
- chest tube drainage
- abdominal drainage / T-Tube drainage / colostomy
- radivac drainage
Other Nursing Procedures ( Daily or PRN )
General dressing
Change of CVP / Arterial line dressings
Change of tracheostomy dressing
Weekly change of CVP / intravenous access / urinary catheter / Ryle’s tube
Weekly hair shampoo
Ø EMERGENCY TROLLEY AND EQUIPMENT
Ø INTUBATION – Preparation of Equipment. Intubation Procedure ( Done by doctor ) Elective or Emergency.
Ø EXTUBATION by nurses accompanied with doctor
Ø ENDOTRACHEAL SUCTIONING
Ø PREPARATION ICU BED
Ø SETTING OF ARTERIAL LINE
Ø SETTING OF CVP LINE
Ø INSERTION OF CHEST TUBE – Preparation of Equipment, Procedure ( To be done by Doctor )- nurses must be observed at wound site and do the dressing.
Ø ENTERNAL FEEDING
Ø TOTAL PARENTERAL NUTRITION ( TPN )
Ø INVESTIGATIONS
Recommended investigations for patient in ICU ,
The blood gas machine in ICU analyses the following:
1. hemoglobin concentration and hematocrit
2. full arterial blood gas analysis
3. Electrolytes i.e. sodium, potassium, chloride and calcium.
Test done in main laboratory.
Test on admission / transferred in
Total white and differential cell count and platelet count only.
Serum creatinine and blood urea.
Blood Sugar ( only in diabetics, severe sepsis, on TPN , liver dysfunction).
CXR ( only intubated patient, pneumonia and chest injury.
Patients requiring postoperative ventilation for few hours need not require CXR routinely ).
Tracheal aspirate culture and sensitivity on intubation.
LFT when indicated, e.g. TPN patients, sepsis.
Coagulation profile when indicated.
Tests ordered daily
1. CXR ( pneumonia or chest injury cases only )
2. RBS ( diabetics, patient on TPN or hypoglycaemic cases.)
3. Other tests when indicated only.
Tests ordered biweekly ( Monday and Thursday )
1. Tracheal aspirate C&S.
2. Serum Calcium / Phosphate / Magnesium.
3. Liver Function Tests.
Other tests when indicated only.
Septic Workout
Ø Blood C&S, urine C&S, tracheal aspirate C&S, swab C&S ( if any wounds ) – results must be traced the following day.
DIC Screening ( send to blood bank )
Ø To get Blood bank Medical Officer approval before sending
- Full Blood Picture
- Full Coagulation Profile
After office hours,
Ø PT/APTT and serum fibrinogen is done in Biochem lab.
Blood sample to be taken from vein or artery and NOT from arterial line ( due to presence of heparin ).
Orthers
Ø Serum lactate ( to get appointment and container )
Ø Serum ammonia ( to get appointment and container from lab.)
Ø Specimen taken to be stored in ice and dispatch immediately
Ø Serum cortisol.
Serum Drug Level
When organ toxic drugs are used e.g. aminoglycosides.
Drugs with narrow therapeutic index e.g.phenytoin, digoxin, aminophylline.
The 1st sample is taken after the 3rd.dose
Post- level : to be taken 1 hr after the dose is given.
Results must be traced by afternoon and / or prior to next dose.
This schedule is to be used as a guideline only. The indication and frequency of relevant investigation is based on severity of illness, progress of patients and changes in treatment modality. All results should be reviewed and upload by the ICU medical officer in the investigations chart as soon as they are traced.
INVESTIGATIONS DONE IN BACTERIOLOGY LAB
1. Blood C&S
2. Tracheal / BAL ( broncho-alveolar lavage) C&S /
3. Acid Fast Bacilli C&S
4. Urine C&S
5. Stool C&S
6. Swab (s) C&S e.g. wound swab C&S.
7. Body fluids C&S e.g. pleural fluid C&S / drainage fluid
8. C&S
9. Spinal fluid C&S
10. Fungal C&S
INVESTIGATIONS DONE IN BLOOD BANK
Blood grouping and cross matching – GXM form
HIV screening }
Hepatitis B.C }
LE ( lupus erythematosus ) cells } Pink haematology form
Coombs’ test }
Hb & Electrophoresis }
Rh factor }
Blood reaction studies – Blood reaction form due to blood transfusion
Serum Japanese B virus
All hormonal studies e.g. serum prolactin level etc.
Histopathological examination ( HPE )
Coxsackie studies
Serum dengue serology
Viral studies
Others as stated from time to time.
COLLECTION OF C&S SPECIMENS
Ø Tracheal Aspirate C&S
Ø Broncho-alveolar Lavage ( BAL ) – To be done by doctor during bronchoscopic suctioning assisted by MA. Specimen will be collected directly to the special C&S container.
Ø Drainage / Pleural Fluids
Ø Urine C&S
Posted by BB at Monday, April 06, 2009 0 comments
Tuesday, March 31, 2009
INFECTION CONTROL & DISEASES DISORDER
INFECTION CONTROL
Nosocomial infection is a major problem in the ICU leading to prolonged stay, increasing morbidity and mortality, and increased coasts.
The following guidelines aim to reduce the transmission of infection:
• Everyone who comes into contact with the patient MUST WASH his or her hands before and after handing the patient. The ICU nurses have given the authority to ensure this practice is carried out.
• All staff should be appropriately gowned, gloved and masked when carrying out invasive procedures.
• To reduce the traffic flow in ICU, the ICU round by doctors of other units should be limited to 4 persons.
NOSOCOMIAL INFECTION CONTROL
GENERAL MEASURES
1. PROPER HAND WASHING before and after each patient contact.
2. Practice aseptic technique for all invasive procedures.
3. Take standard precautions when handling all body secretions.
4. Isolate all infectious patient.
SPECIFIC MEASURES
Venous Lines
1. Insertion under aseptic technique.
2. Apply sterile transparent dressings at insertion sites.
3. Use minimum number of three-way-taps and stop-cocks.
4. Use triple lumen for multiple drug infusion.
5. Inspect the catheter site daily. Avoid blood residue to stagnate in the lines or three-way-tap.
6. Replace lines
• After 5 to 7 days routinely
• Any signs of inflammation at sites
• Any unexplained fever, increased TWDC or sepsis
• If staphylococci is isolated in the blood
7. TPN line must be dedicated line.
Arterial line
1. To be done under aseptic technique.
2. Do not push blood back into the line.
3. Do not allow blood residue to stagnate in line or 3 way tap.
4. Replace line after 5 to 7 days or at any time of signs of inflammation at puncture site.
Urethral Catheterisation
1. To be done under aseptic technique.
2. To use a closed drainage system to collect urine.
3. To remove as soon as possible/weekly change of catheter.
Equipment
1. Ventilator
• Change of ventilator tubings/ humidifier/ resuscitation bag/oxygen apparatus every 48-72 hours.
2. Suction catheters to be used once only.
Suction tubings
• Tip must be covered when not in use.
• To be discarded daily and every new admissions.
3. Suction liner to be discarded when full/every admissions.
4. Wipe surroundings daily and on discharge
• Bed/ mattress / cables/ stethoscope/ monitors / perfusors / drip stand/etc.
Staffing
1. minimize number of visiting doctors/nurses in ICU to 4 doctors per discipline.
2. all ICU staffs to be well-versed with nosocomial infection control protocol.
Visitors
1. Discourage casual visitors
2. Educate close relatives to wash hands before and after touching the patients.
BARRIER NURSING
To be carried out for patients who present a risk to others or vice versa.
1. Nursing patient in isolated area.
• To wear gown and gloves when attending to patient.
• To remove gown and gloves and wash hands before leaving the room.
• The staff in-charge to remain in the isolated room.
2. Minimize visitors.
3. Do not overstock equipment.
• Necessary equipments only to be kept in the room.
4. Linen to be sent separately to laundry unit. Dressings and waste to be disposed according to protocol e.g. to pour hydrogen peroxide before disposal of gas gangrene dressings.
5. Once the room is vacated
• Disinfect and clean the equipments in the room thoroughly.
• To clean and disinfect the room.
• Linen used to pack and label separately before sending to laundry unit.
PROTECTION YOURSELF AND OTHERS
HEALTH HAZARDS ON THE JOB
Tuberculosis , Hepatitis. AIDS. As a healthcare worker in today’s world, it may seem that all you hear about are communicable diseases and the increasing risks they pose to your health.
Although you shouldn’t be overly alarmed, you need to be aware of the risks and the simple ways in which you can avoid them-----to protect yourself as well as your coworkers and patients.
Hidden Dangers
Some health risks in your workplace are obvious. Others are not. Infectious organisms may be anywhere around you. From needle sticks to coughing patients, a variety of accidents and situations can expose you to infection----and lead to life-threatening consequences. How should you deal with these possible dangers? Start by understanding which infectious diseases can be spread in your workplace.
The Risk of Infection
Healthcare workers are at risk of exposure to infectious diseases such as:
Tuberculosis ( TB ), a bacterial infection that effects the lungs, but can also be present in other parts of the body;
Hepatitis B virus ( HBV ), a virus that can cause severe liver damage and even death; and
Human immunodeficiency virus ( HIV ), a virus that causes acquired immunodeficiency syndrome ( AIDS )
Other common health risks in your workplace include hepatitis C, malaria, syphilis, lice, scabies, measles, cytomegalovirus, chickenpox, herpes, ‘staph’ infections, colds, ‘ flu and diarrheal infections. If you suspect that you or a patient has been infected, be sure to report it according to your employer’s policies.
Simple Steps to Protection
Once you are aware of the risks around you, you need to know the steps for preventing exposure to those risks. This booklet will show you how to protect yourself and others against several specific infections by using precautions.
No matter what you come into contact with, two of your best defenses are handwashing and the use of personal protective equipment ( PPE )-----specialized clothing or equipment worn for protection against hazards.
Wash Your Hands Often
Removing germs by handwashing provides vital protection against many types of infection. Always wash your hands before and after you have contact with a patient or anything a patient has touched.
Remember the following:
Wash your hands immediately after removing gloves---and before eating, drinking , smoking, applying makeup or handling contact lenses.
Work up a good lather with nonabrasive soap and running water. Clean between your fingers and around your nails. Then rimes well.
If your hands or any other part of your body fluids, immediately wash exposed skin thoroughly.
Use PPE ( Personal protective equipment )
Designed to protect you from a variety of hazards, PPE helps guard your skin, eyes, mouth and personal clothing from exposure to infectious germs. Your employer will provide the type of PPE that is most effective for your particular job. Never wear PPE that’s damaged or soiled. After use, remove PPE and palace it in the proper container for cleaning, decontamination or disposal.
TUBERCULOSIS
An infectious disease that usually begins in the lungs, TB may spread to the brain, kidney or spine. Most people who are infected with TB will never develop the active disease, but the disease can develop at any time if it is not treated with medication.
How TB Infection Occurs
TB can be spread when a person with active TB disease coughs, shouts, or laughs, spraying bacteria-contaminated droplets into the air. The infection is most likely to be spread in small, poorly ventilated rooms, and usually results from prolonged exposure.
Inactive TB
In most people, infectious TB bacteria remain inactive for a lifetime---their immune systems prevent the infection from progressing. A person who is infected with inactive TB isn’t sick, doesn’t have symptoms, and can’t infect others. In fact, the only way to know if you’ve been infected is to get tested. That’s why it’s vital for healthcare workers to have a TB skin test once or twice a year. If you are infected, medication can help ensure that you will not develop active disease.
Active TB
Inactive infection becomes active disease if the TB bacteria grow and begin to attack a body organ, often the lungs. Symptoms may include persistent coughing, fatigue, weight loss, fever, loss of appetite and night sweats. If left untreated, TB can be fatal. Fortunately, when taken properly, medication can completely cure the disease. People who stop their medications or who take them irregularly may develop drug-resistant TB, which is sometimes impossible to cure.
Using the Right PPE
When working in or visiting areas with suspected or confirmed cases of TB, use appropriate masks, such as HEPA ( high-efficiency particulate air ) filter respiratory masks or dust-fume-mist masks. Your employer’s respiratory protection policy may recommend other types of PPE, as well.
Controlling TB
You and your facility can use a variety of methods to limit the spread of TB:
• Place TB patients in negative-pressure isolation rooms with a minimum of six air changes per hour ( preferably 10 – 12 air changes per hour ).
• Ask TB patients to cover their noses and mouths with tissue when they cough or sneeze. When transporting TB patients outside of their rooms, be sure they wear surgical masks.
• Use a HEPA filter hood to prevent the spread of TB germs when inducing and collecting sputum.
BLOODBORNE PATHOGENS
Whether or not you work directly with patients, you need to protect yourself from expose to bloodborne pathogens ie, disease-causing germs carried by blood or certain body fluids. Knowing how these infections are spread will help you prevent them.
How Bloodborne Diseases Are Spread
Many infectious germs are carried in blood and in other body fluids in which blood may be present such as saliva, semen, fecal matter, and amniotic fluid. If infected blood comes into contact with any opening or break in your skin, you may be exposed to disease. Two of the most common and dangerous types of bloodborne disease that may infect healthcare workers are caused by the hepatitis B virus ( HBV ) and the human immunodeficiency virus ( HIV ).
HBV
HBV infection can lead to liver damage, cancer ,and even death. Symptoms may be mild and flulike. Some people have no symptoms are all.
A vaccination series is available to prevent hepatitis B infection. Your employer provides the hepatitis B vaccination free of charge to employees who are at risk for bloodborne exposure. HIV
Although HIV is much less likely than hepatitis B to be spread in the workplace, it could potentially be spread anywhere that blood is present. HIV weakens the body’s immune system and causes AIDS. Symptoms may include weight loss, night sweats, fever, fatigue, gland pain and swelling, and muscle or joint pain. There is currently no vaccine for HIV and no cure for AIDS. Other Bloodborne Diseases
Blood may carry other serious infections, such as hepatitis C, malaria , and syphilis. If discovered early enough, these conditions can usually be treated with medication.
Exposure Control Plan
Your employer’s exposure control plan is a document that describes when or where an exposure could occur, standard precautions, exposure reporting procedures, and training requirements. You have the right to see that plan at any time. Ask your supervisor for more information.
Standard Precautions
The idea behind standard precautions is simple but effective: Since you don’t always know whose blood is carrying infectious germs, treat all blood and certain body fluids as potentially infectious. Protective controls to help you avoid bloodborne hazards include the following:
Engineering controls, such as safely mounted sharps containers, are your company’s technological means of isolating or removing hazards from the workplace to reduce your exposure to blood.
Work practice controls, such as avoiding contact with blood, are ways that you can perform your job more safely to prevent exposure to bloodborne pathogens
Engineering Controls
By making the work environment safer, your employer can greatly reduce your risk of exposure to bloodborne infections. Sharps containers and medical safety devices are examples of protective engineering controls.
Sharps Containers
Immediately after using sharps, dispose of them in containers are:
• Puncture-resistant
• Leak proof on sides and bottom
• Labeled or color-coded as biohazardous
• Closable
• Located in areas that can be safely and conveniently reached
Safer Medical Devices
Many needles and other medical instruments now have safety features to help prevent accidents and exposure to disease. These devices include:
• Self – sheathing needles
• Needless IV connectors or connectors with recessed needles
• Phlebotomy devices and lancets with safety features such as retractable blades
• Face masks used for mouth – to – mouth resuscitation or cardiopulmonary resuscitation ( CPR )
Work Practice Controls
Engineering controls alone won’t do much good unless you follow safe work practices. Proper waste disposal, safe needle handling and thorough cleaning are a few important ways to help ensure on – the – job safety.
Marking Infectious Materials
Any potentially infectious materials must be labeled or color – coded as biohazardous. Labels must also be placed on cabinets, refrigerators, freezers or any other containers holding blood or other potentially infectious materials.
Disposing of Waste
Whether you’re disposing of used needles, blood-stained towels, tissue specimens, or other contaminated materials, always follow your facility’s waste disposal guidelines. All medical waste should be stored in labeled, closed containers that can hold the contents without leakage during handling, storage, and transportation.
More Work Practice Controls
Handling Needles
One of the most important ways to prevent exposure to infection is to handle needles carefully. Keep the following guidelines in mind.
• Never bend or break needles;
• Never remove needles from disposable syringes;
• Do not recap needles. If you do, use an approved recapping method.
• Always dispose of needles in proper sharps containers.
• If a needlestick occurs, wash the affected area thoroughly with soap and running water. Then report it according to your employer’s policies.
Removing Gloves
To prevent contact with any blood that may be on your gloves, remove them carefully, using the following steps:
Peel one glove off from wrist to fingertips and hold it in the other, gloved hand.
Peel the other glove off from the inside with your exposed hand, holding the first glove inside the second.
Properly dispose of the gloves. Then wash your hands thoroughly.
Staying Aware
Throughout the working day, pay attention to your activities and your environment. Do not eat, drink, apply cosmetics, or handle contact lenses in patient care areas of possible contamination.
Housekeeping
When cleaning any contaminated materials or surfaces, remember the following:
• Wear gloves and protective covering over your clothing.
• When cleaning up blood spills, use disposable towels and an approved disinfectant. Dispose of waste properly. If splashing may occur, wear protection for your eyes and face.
• Separate contaminated laundry into leak proof, biohazard-labeled bags or containers.
UNIVERSAL PRECAUTIONS
Hospital staff must use precautions with blood and body fluids from all patients to protect themselves from blood borne pathogens.
These precautions also protect against other infectious organisms.
All patients are to be treated as potential source of infection e.g. HIV, Hepatitis B etc.
Wash hands before and after all patients or specimen contact. Proper handwashing with ordinary soap and water is sufficient except for invasive procedures when antiseptic soap is necessary.
Handle the blood and body fluids of all patients as potentially infectious.
Wear gloves for potential contact with blood and body fluids or when there is direct contact with non-intact skin or mucous membrane.
Place used syringes immediately in nearby 100% puncture resistant container, do NOT recap or manipulate needle in any way.
Wear protective eyewear and mask if there is a possibility of splatter with blood or body fluids ( e.g. bronchoscopy, oral surgery )
Wear gowns or apron when splash with blood or body fluids is anticipated.
Handle all linen soiled with blood and/or body secretions as potentially infectious.
Process all laboratory specimens as potentially infectious. Autoclave/heat treat where necessary before disposing.
Any spillage should be treated with 0.5-1% sodium hypochlorite before cleaning.
Wear masks for protection against airborne infections.
It takes up to six months after exposure for a person to develop HIV antibodies.
INVASIVE MONITORING [ PART TWO ]
Background
Invasive pressure monitoring systems are widely used for bedside monitoring of hemodynamic changes in the critically ill patients.
One component of an intravascular monitoring system is a fluid-filled catheter, one end of which is placed within the vascular system. The catheter is connected to a transducer, which is an electronic device that converts physiological events
( alternation in pressure ) to electronic signals that can be displayed on an oscilloscope. To ensure accuracy and to allow for changes in atmospheric pressure, the transducers are periodically balanced and recalibrated. When measuring pressures, the transducer should be positioned at the level of the cardiac chamber in which the catheter tip is positioned. Too high a position of the transducer will results in erroneous low reading. A falsely high reading will results if the transducer is placed too low because of hydrostic pressure on the transducer. For accurate monitoring the transducer should be positioned at the phlebostatic axis, which is measured from the fourth intercostal space in the midaxillary line, which corresponds to the level of the right atrium. Mark this point with a magic marker to establish a consistent 0 reference point.
Use a carpenter’s level to check the position of the transducer in relation to the mark on the chest. Reading can be taken in any position, although the supine position is preferred. Take serial readings in the same position.
A variety of equipment is used for pressure monitoring and much of this equipment is disposable. A continuous low-pressure flush systems is used to prevent clot formation within arterial catheter. Clot formation inhibits free transmission of the pressure waves and increases the risk of embolisation.
To minimize the risk of comtamination or air leaks and to increase accuracy, use high pressure tubing with as few connections and stopcocks as possible.
Haemodynamic Parameters
Haemodynamic parameters that are commonly used to assess critically ill patients include the peripheral arterial pressure, central venous pressure, pulmonary artery wedge pressure, cardiac output and mixed venous oxygen saturation.
Continuous arterial pressure is monitored by cannulating a peripheral artery by using an intravenous
( IV ) cannula and connecting to the transducer system. An arterial waveform is displayed on the oscillioscope if the system is free of air bubbles, clots and kinks.
The normal range for arterial pressure in adults :-
Systolic pressure : 100mmHg – 140mmHg
Diastolic pressure : 60mmHg - 80mmHg
Mean arterial pressure (MMP ) 70mmHg – 90mmHg
Ø TRANSDUCER SETUP – To continuously monitor a single pressure or two pressures alternatively.
Ø ARTERIAL LINE – Insertion of a cannula into the artery. To maintain continuous beat monitoring of blood pressure in the critically ill patient. To obtain repeated arterial blood samples with minimal discomfort to the patient.
- Reference Point
- Arterial monitoring Setup
Ø CENTRAL VENOUS PRESSURE – is a measurement of the volume status of patient. It also indicates the competence of the right heart to accept and expel the blood returned. It assesses how well the right ventricle functions as a pump. It can be measured using either a simple fluid manometer or a transducer.
- To assess haemodynamic changes occurring in the right side of the heart.
- To administer fluids or medications directly to the central veins.
- To obtain central venous blood samples.
- To assess volume status of a patient in shock and the response to treatment.
- To provide an early recognition of congestive cardiac failure ( CCF ).
Note:-
Avoid using subclavian approach in patients with coagulopathy as it would be difficult to control any bleeding, especially if subclavian artery is inadvertently punctured.
Ø PULMONARY ARTERY (SWAN – GANZ ) CATHETER – Pulmonary Artery Pressure ( PAP ) is measured using a balloon tip flow directed catheter.
- To measure intracardiac pressures e.g. CVP, PAP, PAWP
- To measure cardiac output and derived variables ( SVR, PVR)
- For mixed venous blood sampling
- For cardiac pacing.
Ø NON – INVENSIVE MONITORING – Blood Pressure – Manually ( Sphygmomanometer and stethoscope ) . Electronic / automatic – DINAMAP. Monitoring peripheral pulse using DOPPLERS ‘ ultrasound.
Ø MONITORING PERIPHERAL PULSES USING DOPPLER ULTRASOUND – techniques can be used to amplify and assess peripheral blood flow. Transmitting crystals in the probe emit ultrasound beams that collide with red blood cells moving through the blood cells to a receiver.
The change in sound is converted into an audible sound that is amplified to be heard. If the blood flow is less than 5 cm per second or is shielded by bone, or is located deep below the skin surface, it cannot be heard.
- to assess blood flow in peripheral vessels
- to diagnose peripheral vascular disorders.
- To amplify the blood pressure when it cannot be auscultated using traditional methods.
MECHANICAL VENTILATION ( PART THREE )
Introduction
A large number of patients in ICU are unable to maintain adequate ventilation. They will require the use of ventilatory support. It is thus essential that the nurse caring for these patients have a basic working knowledge on ventilator function and management of ventilated patient.
Principles of Mechanical Ventilation
Spontaneous of normal ventilation will establish airflow into the lungs by creating negative pressure
Within the thoracic cage. This negative pressure occurs when the respiratory muscles expand and slightly raise the ribs, while stimultaneously lowering the diaphragm. The net effect is an increase in the intrathoracic volume which is associated with an increased negative pressure.
Air is then automatically ‘ sucked’ in to fill this space. The larger the space created, the greater the volume of air that is drawn in.
These explains our ability to vary the size of our inspirations from those of a huge sigh to shallow, quiet breathing. Conversely, inspiration during the mechanical ventilation is achieved by means of positive pressure. The gas is driven into the lungs by an external force, i.e. the mechanical ventilator. In both spontaneous and mechanical ventilation, expiration is passive i.e. it depends on the elastic recoil of the lungs.
This illustrates the difference in intrathoracic pressure changes during spontaneous ventilation and mechanical ventilation. It is important to understand the fundamental difference here as it is the key to identifying and predicting potential problems for the mechanically ventilated patients.
Types of Positive Pressure Ventilators
Positive pressure ventilators inflate the lungs with a positive pressure ( compare normal breathing where inspiration is by a negative airway pressure ) then, allow expiration to occur to the atmosphere by the natural elastic recoil of the lungs and the chest wall.
2 most common types of ventilators used in adult critical care are:-
Ø Volume cycle ventilators
Ø Pressure cycle ventilators
Mode of Ventilation
1. Controlled Mandatory Ventilation ( CMV )
Is provided regardless of the patient’s ability to breathe. The major disadvantage is that the ventilator is totally unresponsive and independent of patient’s effort or responses.
2. Assist / control
Patient’s initiated breaths will receive the same preset tidal volume as ventilator initiated breaths.
3. Intermittent Mandatory Ventilation ( IMV )
It is a controlled mode ( with a low preset rate ) which allows spontaneous breathing in between controlled breaths. The two breathing patterns ( ventilator and Patient ) are not synchronized.
4. Synchronized Intermittent Mandatory Ventilation ( SIMV )
The patient breaths through a circuit that allows for independent spontaneous ventilation and the mandatory ventilator breaths ( which are triggered by the patient ) or synchronized to the patients breaths.
5. Pressure Support
Is spontaneously breathing mode, and if the patient does not make an inspiratory effort, apnea will occur. This mode is usually for weaning the patient from the ventilator because the patient must initiate breaths ( by creating a negative pressure to the patient by trigger value ) and pressure support assists the patient by delivering a flow of gas up to the preset pressure level.
6. PEEP / CPAP
Positive End-Expiratory Pressure ( PEEP ) is a maneuver used during IPPV where a prescribed pressure is applied during expiration so that a minimum positive pressure always occur during expiration. The aim is to maintain a minimum positive intrapulmonary pressure throughout the respiratory cycle.
COMPLICATION OF MECHANICAL VENTILATION
1. Mechanical – equipment malfunction
2. Physiological
a) Respiratory – barotraumas , atelectasis , infection
b) Cardiovascular – decreased venous return and cardiac output
c) Gastrointestinal – gastric ulcerations, micro aspirations
d) Renal / Hepatic – decreased urine output, sodium and water retention, decreased portal blood flow
e) CNS – decreased cerebral perfusion pressure following excessive PEEP
NURSING MANAGEMENT OF VENTILATED PATIENTS
Nursing Responsibilities can be grouped into 3 basic sections :-
1. Assessment and monitoring of the patients physical status and haemodynamic parameters.
2. Monitoring the ventilation parameters. The nurse should be able to recognize and trouble-shoot ventilator problems.
3. Nursing care. This includes skills such as suctioning via ETT, repositioning and securing an ETT, use of artificial airways. ( See airway management )
It must be emphasized that the most important monitor is the nurse.
Patient on life support system such as a ventilator should never be left unattended because failure of the system or development of life threatening complications such as pneumothorax may occurs.
The nurse must be alert to any sudden changes in system performance, or any acute development, distress, cyanosis, tachycardia and unequal breath sounds in the patient. When ventilation is completely controlled with sedation and paralysis, nursing will be the same as that of an unconscious patient.
The nurse must assume the protective reflexes for the patient until he is aware of himself and can function in his own. Patient communication is important and he must always be spoken to as if he is awake. A brief explanation should be given prior to any procedure to be performed.
1. OBSERVATION
1.1 PATIENT :-Conscious state, Colour ,BP, Pulse, Respiratory Rate, CVP
- Chest movement , Oxygen Saturation ( SpO2 )
1.2 VENTILATOR :- Mode , FiO2 , Set tidal volume , Rate , Airway pressure , Airway temperature
2. Alarm limits be set appropriately. Apnea alarm must NEVER be disabled.
3. Disconnection from ventilator requires IMMEDIATE reconnection.
4. in event of machine failure or power failure, commence manual ventilation immediately. Therefore a self-inflating bag with oxygen source must always be available at every bed.
5. drugs may be necessary when the patient is unable to settle with reassurance and inadequate ventilation.
Drugs used in management of ventilated patients
Commonly used drugs include:
Sedatives / analgesics
- Midazolam
- Morphine
- Propofol
Neuromuscular Blocking Agent ( NMBA )
- Suxamethonium ( Scoline )
- Vecuronium ( Norcuron )
- Atracurium ( Tracium )
The use of NMBA in the management of patients on a mechanical ventilator has decreased over the years. They are usually reserved for patients who are more difficult to settle and during the initial stages of stabilization, and for cerebral protection of patients with very high intracranial pressure ( ICP ).
It is important to remember that muscle relaxants have no sedative and analgesic effects – the patient can still hear and experience pain but will be unable to respond . therefore they must be adequately sedated while on muscle relaxants.
WEANING OF MECHANICAL VENTILATION
The process of weaning off the ventilator implies a gradual withdrawal of mechanical ventilatory support. It may take a number of forms and is affected by a number of physiological factors.
Factors To Consider Before weaning
1. Resolution of underlying pathologic condition initially requiring ventilatory support.
2. CXR shows good lung expansion and clear lung fields.
3. Acceptable ABGs with low ventilatory support.
4. Sepsis under control.
5. Awake with intact respiratory drive.
6. Minimal inotropic support.
7. Good hydration status with normalized serum electrolytes electrolytes and acid base status.
8. Adequate nutrition and energy.
9. Intact gag and cough reflex before extubation
Respiratory Criteria for Weaning
PARAMETER CRITERIA
Respiratory Rate 8 – 25 / min.
Vital Capacity 10 – 15 ml / kg
Maximum Inspiratory Force > - 20 cm H2O Pressure
PaO2 > 80 mm hg with FiO2 <>
PaCO2 35 – 45 mm hg
( except in cases of chronic hypercapnia )
Tidal Volume > 5 ml / kg
Posted by BB at Tuesday, March 31, 2009 0 comments
Saturday, March 28, 2009
HISTORY OF NURSES
Sense of Belonging - Ownership – security usage and maintenance
Sense of Guilt - Aware and realize the effect of failure for not fulfilling expectations or observing correct form guideline or procedures
Sense of Sin - Realized , acknowledge and regret of whatever wrong doings.
Sense of Shame - Having strong believe in protecting and preserving self – esteem and self – pride from moral decadence as a result of wrong doings ( written and unwritten rules and practices )
Pioneer Nurses of West Virginia
Pioneer Nurses of West Virginia, the first online to honor the Pioneer Nurses of West Virginia, is in conjunction with my other West Virginia sites that memorialize our ancestors, as well as the history of West Virginia.
For the purposes of this website, the Pioneer Nurses are those who were nurses in
Also included here are the nurses from
But this site will NOT be limited to only those nurses (pre-1935) who were "registered." There were MANY early nurses who practiced as nurses but were never licensed. Some graduated from organized schools of nursing and others studied under a physician. Legally, if they didn't get a license when it became a requirement, they weren't registered nurses - - but they were, indeed, nurses. They will be included in a separate section.
Visitors to this site are invited to submit photos and biographies of the nurses.
Submitted by
Linda Cunningham Fluharty RN.
 The Zwerdling Nursing Archives
The Zwerdling Nursing Archives
The History of Nursing Education
Nursing Schools in Nova Scotia
 At first enrolments in nursing schools were very small, but by the beginning of the twentieth century it became apparent that the hospital trained nurse would dominate the field and the number of nursing schools and nursing students quickly increased. The greatest expansion of nursing schools in
At first enrolments in nursing schools were very small, but by the beginning of the twentieth century it became apparent that the hospital trained nurse would dominate the field and the number of nursing schools and nursing students quickly increased. The greatest expansion of nursing schools in
Hospital administrators immediately began to recognize the improvements the trained nurses were making to patient care, and began to replaced their untrained nursing staff with student nurses, who spent two or three years working in the hospital wards in exchange for training and certification. This system of staffing hospitals and training nurses not only enabled the
Posted by BB at Saturday, March 28, 2009 1 comments
PROFESSIONAL DEVELOPMENT OF NURSES
Nursing involves the giving of care to the patients together with other members of the health care team including doctors. The person in the centre of these activities is a biopsychososial being called the PATIENT. Nurses exist because of these important individuals – THE PATIENTS.
A PROFESSIONAL NURSE is one who works with her patients at the highest level of knowledge, skills and a caring attitude while adhering to a set of code of ethics.

Of importance in the definition are:
1. Highest level – best of the highest possible standards.
2. Knowledge – Need to be aware of advances in knowledge and technologies in medical sciences.
3. Skill – Competency in the various skills required in nursing.
4. Caring attitude – Recognizing the need of the patient to be managed with compassion, courtesy, respect and dignity.
5. Code of ethics – A set of rules to guide professional behaviour.
All the above are ingredients of the professional development of a nurse.
The early professional development of a nurse is initiated by training schools but it does not end here. Professional development is a continuous process in the nurses career. This is important if we nurses are to gain respect and recognition.
There is a need for the nurse to be assertive and to function as an equal member of the health care team. This would become possible if she develops appropriately in the following three arrears:
KNOWLEDGE
SKILLS
ATTITUDES
Background
1. The level of care provided in a general intensive care unit (ICU) is more complex than delivered in a general ward.
2. It is about 3.8 times more expensive to maintain ICU than a general ward.
3. currently, in United States the provision of ICU costs about 15% of the total hospital care.
4. Level of ICU care defers from hospital to hospital in Malaysia, according to facilities available.
5. In Malaysia managing an ICU bed cost about RM 2,000/ per day compared to an ordinary 3rd class bed which costs about RM200/per day.
Philosophy
The philosophy of the unit is that each patient is a person with a unique human dignity for whom medical personnel assume the responsibility of giving comprehensive, safe, effective medical & nursing care and protection.
Objectives
To provide directions in the nursing management of ICU.
To develop protocols and guidelines in the running of ICU since it demands an extensive commitment of time, manpower, equipment and money.
To manage critically ill patients with potential reversible pathology who require intensive monitoring and life support system.
To provide training and skills for medical and paramedical staffs in the field of critical care.
Our vision
To provide nursing knowledge that can be applied in the clinical setting when caring for real people.
Reflect current knowledge of the science and art of nursing in today’s world.
Provide clear explanations of the pathophysiologic processes of various disorders.
Emphasize the nurse’s role in collaborative care.
Prioritize nursing interventions specific to altered human responses to illness.
Foster critical-thinking skills
Offer visual tools for learners
Posted by BB at Saturday, March 28, 2009 0 comments










